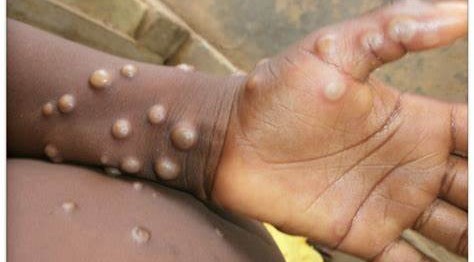
Mpox patient presenting rash symptoms - Courtesy
South Sudan has not yet recorded a case of Mpox formerly known as monkeypox, according to the Ministry of Health, but the virus has been a public health concern in Africa for decades, and is currently spreading in the east African region, particularly in the Democratic Republic of Congo.
On August 14, a new strain of the Mpox virus named ‘clade 1b’, which has caused over 18,000 suspected cases and 615 deaths in DR Congo this year, was declared a health emergency by World Health Organization (WHO).
South Sudan is on high alert after the new strain was recorded among some of its neighbors including Kenya, Uganda, DRC, and Central Africa Republic.
Mpox is an infectious disease that can cause a painful rash, enlarged lymph nodes, fever, headache, muscle ache, back pain and low energy. Most people fully recover, but some get very sick.
It is caused by the monkeypox virus (MPXV) and is an enveloped double-stranded DNA virus of the Orthopoxvirus genus in the Poxviridae family, which includes variola, cowpox, vaccinia and other viruses, according to WHO.
The UN health agency and scientists have identified two distinct clades of the virus: clade I (with subclades Ia and Ib) and clade II (with subclades IIa and IIb).
A global outbreak of clade IIb began in 2022 and continues to this day, including in some African countries. There are also growing outbreaks of clades Ia and Ib affecting the DRC and other countries in Africa. As of August 2024, clade Ib has also been detected beyond Africa.
The natural reservoir of the virus is unknown, but various small mammals such as squirrels and monkeys are susceptible.
Mpox is said to spread from person to person mainly through close contact with someone who has mpox, including members of a household.
Close contact includes skin-to-skin (such as touching or sex) and mouth-to-mouth or mouth-to-skin contact (such as kissing), and it can also include being face-to-face with someone who has mpox (such as talking or breathing close to one another, which can generate infectious respiratory particles).
People with multiple sexual partners are at higher risk of acquiring mpox.
People can also contract mpox from contaminated objects such as clothing or linen, through needle injuries in health care, or in community settings such as tattoo parlours.
During pregnancy or birth, the virus may be passed to the baby. Contracting mpox during pregnancy can be dangerous for the fetus or newborn infant and can lead to loss of the pregnancy, stillbirth, death of the newborn, or complications for the parent.
Animal-to-human transmission of mpox occurs from infected animals to humans from bites or scratches, or during activities such as hunting, skinning, trapping, cooking, playing with carcasses or eating animals. The animal reservoir of the monkeypox virus remains unknown and further studies are underway.
More research is needed on how mpox spreads during outbreaks in different settings and under different conditions.
Mpox causes signs and symptoms which usually begin within a week but can start 1–21 days after exposure. Symptoms typically last 2–4 weeks but may last longer in someone with a weakened immune system.
Common symptoms of mpox are: rash, fever, sore throat, headache, muscle aches, back pain, low energy and swollen lymph nodes.
Some people also have painful swelling of their rectum (proctitis) or pain and difficulty when peeing (dysuria) or when swallowing.
People with mpox can pass the disease on to others until all sores have healed and a new layer of skin has formed. Some people can be infected without developing any symptoms. Although getting mpox from someone who is asymptomatic (not showing symptoms) has been reported, information is still limited on how common it is.
Children, pregnant people and people with weak immune systems, including people living with HIV that is not well controlled, are said to be at higher risk for serious illness and death due to complications from mpox.
Identifying mpox can be difficult because other infections and conditions can look similar. It is important to distinguish mpox from chickenpox, measles, bacterial skin infections, scabies, herpes, syphilis, other sexually transmitted infections, and medication-associated allergies.
Someone with mpox may also have another sexually transmitted infection at the same time, such as syphilis or herpes. Alternatively, a child with suspected mpox may also have chickenpox. For these reasons, testing is key for people to get care as early as possible and prevent severe illness and further spread.
The preferred laboratory test for mpox is detection of viral DNA by polymerase chain reaction (PCR). The best diagnostic specimens are taken directly from the rash – skin, fluid or crusts – collected by vigorous swabbing.
In the absence of skin lesions, testing can be done using swabs or the throat or anus. Testing blood is not recommended. Antibody detection methods may not be useful as they do not distinguish between different orthopoxviruses.
HIV testing should be offered to adults with mpox, and children as appropriate. Diagnostic tests for other conditions should be considered where feasible, for example, varicella zoster virus (VZV), syphilis and herpes.
The goal of treating mpox is to take care of the rash, manage pain and prevent complications. Early and supportive care is important to help manage symptoms and avoid further problems.
Getting an mpox vaccine can help prevent infection (pre-exposure prophylaxis). It is recommended for people at high-risk of getting mpox, especially during an outbreak.
Groups that may be at high risk of mpox include:
The vaccine can also be administered after a person has been in contact with someone who has mpox (post-exposure prophylaxis).
In these cases, the vaccine should be given less than 4 days after contact with someone who has mpox. The vaccine can be given for up to 14 days if the person has not developed symptoms.
Some antivirals have received emergency use authorization in some countries and are being evaluated in clinical trials. To date, there is no proven effective antiviral treatment for mpox. It is a priority to continue evaluation of therapeutics in robust clinical trials and to focus on optimizing supportive care for patients.
Health experts advise that individuals with HIV and mpox should continue taking their antiretroviral therapy (ART). ART should be initiated within 7 days of diagnosis of HIV.
To prevent spread of mpox to others, people with mpox should isolate at home following guidance from their health care provider, or in hospital if needed, for the duration of the infectious period (from onset of symptoms until lesions have healed and scabs fall off).
Covering lesions and wearing a well-fitting mask when in the presence of others may help prevent spread. Using condoms during sex will help reduce the risk of getting mpox but will not prevent spread from skin-to-skin or mouth-to-skin contact. If having sex, use condoms as a precaution for 12 weeks (about 3 months) after you have recovered.
Taking a break from sexual activity with new partners during periods of increased transmission can reduce the risk of getting mpox.
Those who have had contact with someone with mpox should monitor for signs and symptoms for 21 days (3 weeks) and take precautions such as avoiding sexual activity during this period.
Health workers should follow infection prevention and control measures to protect themselves while caring for patients with mpox by wearing appropriate personal protective equipment (PPE) (i.e. gloves, gown, eye protection and respirator) and adhering to protocol for safely swabbing lesions for diagnostic testing and handling sharp objects such as needles.
The first reported human case of mpox was a nine-month-old boy in the Democratic Republic of the Congo (1970).
Following the eradication of smallpox in 1980 and the end of smallpox vaccination worldwide, mpox steadily emerged in central, east and west Africa.
In 2003, an outbreak in the US was linked to imported wild animals (clade II), and since 2005, thousands of cases were reported in the DRC every year, while in 2017, mpox re-emerged in Nigeria and continues to spread across the country and in travellers to other destinations.
In May 2022, an outbreak of mpox appeared suddenly and rapidly spread across Europe, the Americas and then all six WHO regions.
The global outbreak has affected primarily (but not only) gay, bisexual, and other men who have sex with men and has spread person-to-person through sexual networks. More information on the global outbreak is available here, including information on community responses to control the outbreak.
WHO says stigma and discrimination for any disease are never acceptable, and underscores that stigma linked to mpox can undermine public health efforts or prolong a disease outbreak, as people may be more reluctant to come forward and seek care and treatment.
For mpox, stigma, discrimination and racism have been particularly directed against communities initially most affected by the disease, namely men who have sex with men, trans people and gender diverse communities.
Note: Some information in this story was adapted from the World Health Organization.
Support Eye Radio, the first independent radio broadcaster of news, information & entertainment in South Sudan.
Make a monthly or a one off contribution.
Copyright 2026. All rights reserved. Eye Radio is a product of Eye Media Limited.